Conducting a consultation
What it is: A structured, workflow that guides you through capturing symptoms, recording examination findings, diagnosing, prescribing, and planning patient outcomes, all within a single unified interface.
Why you use it: To replace manual note-writing with a faster, structured process, templates and AI assistance handle the documentation so you can focus on the patient in front of you rather than your screen.
When you use it: Every time a patient is ready to be seen. Open the patient file from your calendar or via search, then click 'Start consult' to begin.
Steps
Step 1: Find the patient on your schedule or search for them
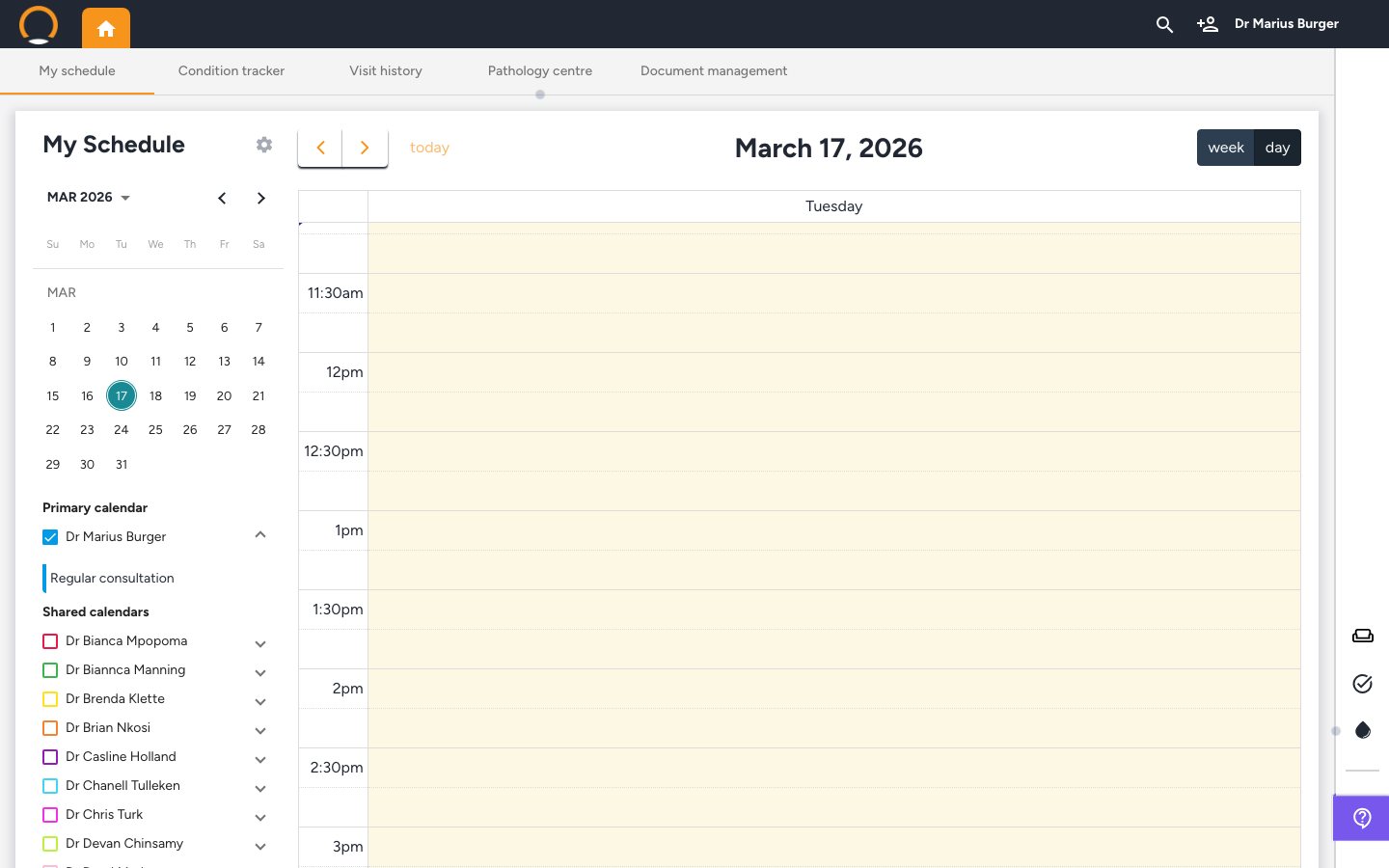
Top navigation bar — patient search bar, Waiting Room, or home dashboard — My Schedule
From the home dashboard, you can open a patient file three ways:
- From My Schedule: Click on the patient's appointment block in the calendar to open their file directly.
- From the Waiting Room: Click the Couch icon in the navigation bar to see patients who have checked in and are ready to be seen. Click a patient's name to open their file.
- From patient search: Click the magnifying glass icon in the top navigation bar, type the patient's name, and select them from the results that appear.
✓ You should see: the Patient overview opens, showing the patient's history, conditions, medications, and patient timeline.
Step 2: Review the patient overview, then click Start consult
Patient file — Patient overview
Before starting, review the pre-consultation information: family members, conditions, medications, and the patient timeline. Use these tools in the Patient Overview to prepare:
- View Summary — click the orange 'View Summary' button next to the patient's name at the top of the Patient Overview. An AI-generated executive summary appears in a pop-up, covering chronic conditions, top care gaps, and upcoming screening opportunities. Click 'Close and Submit' when done.
- Lab History — click the Blood Drop icon in the right-hand panel for a quick view of the patient's recent pathology results. See the Pathology Centre guide for the full workflow.
- Talking Points — a curated list of personalised conversation starters and care prompts for this patient, displayed in the left column of the patient file. Review these before the patient enters to guide a more targeted discussion.
- Clinical Assistant panel (💡) — click the Lightbulb icon next to the 'Patient overview' heading to open (or close) the Clinical Assistant panel on the right side of the screen. The panel has two sections:
- Generate documents — quick access to all five AI document generators (Visit Summary, Custom Document, Medical History Summary, Motivation Letter, Referral Letter) without needing to be inside a consultation. Click any generator to open the Clinical Assistant pop-up and produce a document from the patient's file at any time.
- Get Clinical Insights — click 'Clinical Insights' to open an AI chat interface. Type a specific question about the patient's history (e.g. "What was the last HbA1c result?" or "Has this patient been treated for recurring UTIs?") and click 'Generate'. The AI searches the entire patient timeline and returns a targeted, evidence-based answer. This panel stays accessible during the consultation — use it at any point to query the patient's history without leaving the screen you are on.
When you are ready to begin, click the orange 'Start consult / Continue consult' button in the top-right area of the patient file.
✓ You should see: the consultation opens and you see six tabs across the top: Clinical Notes, Symptoms, Examination, Diagnose & prescribe, Plan, and Review. The Cancel, Save, and Finish buttons appear on the right.
Step 3: Capture clinical notes on the Clinical Notes tab
Consultation — Clinical Notes tab
The 'Clinical Notes' tab opens by default. You can:
- Type manually in the notes field labelled 'Capture general clinical notes'.
- Use Nora — Speech to Clinical Notes (🎤) — click the Microphone icon in the right-hand sidebar to activate Nora, the AI ambient documentation tool. Choose a recording mode:
- Consultation Mode — records the entire patient conversation in the background. Nora listens to both you and the patient and automatically structures the conversation into a clinical note when you stop recording.
- Dictation Mode — you speak a summary or key points yourself (up to 3 minutes) after the fact, and Nora converts it into structured notes. Use this if you prefer to recap after the patient leaves.
- Use a template — click the template icon in the toolbar to insert a pre-saved notes template.
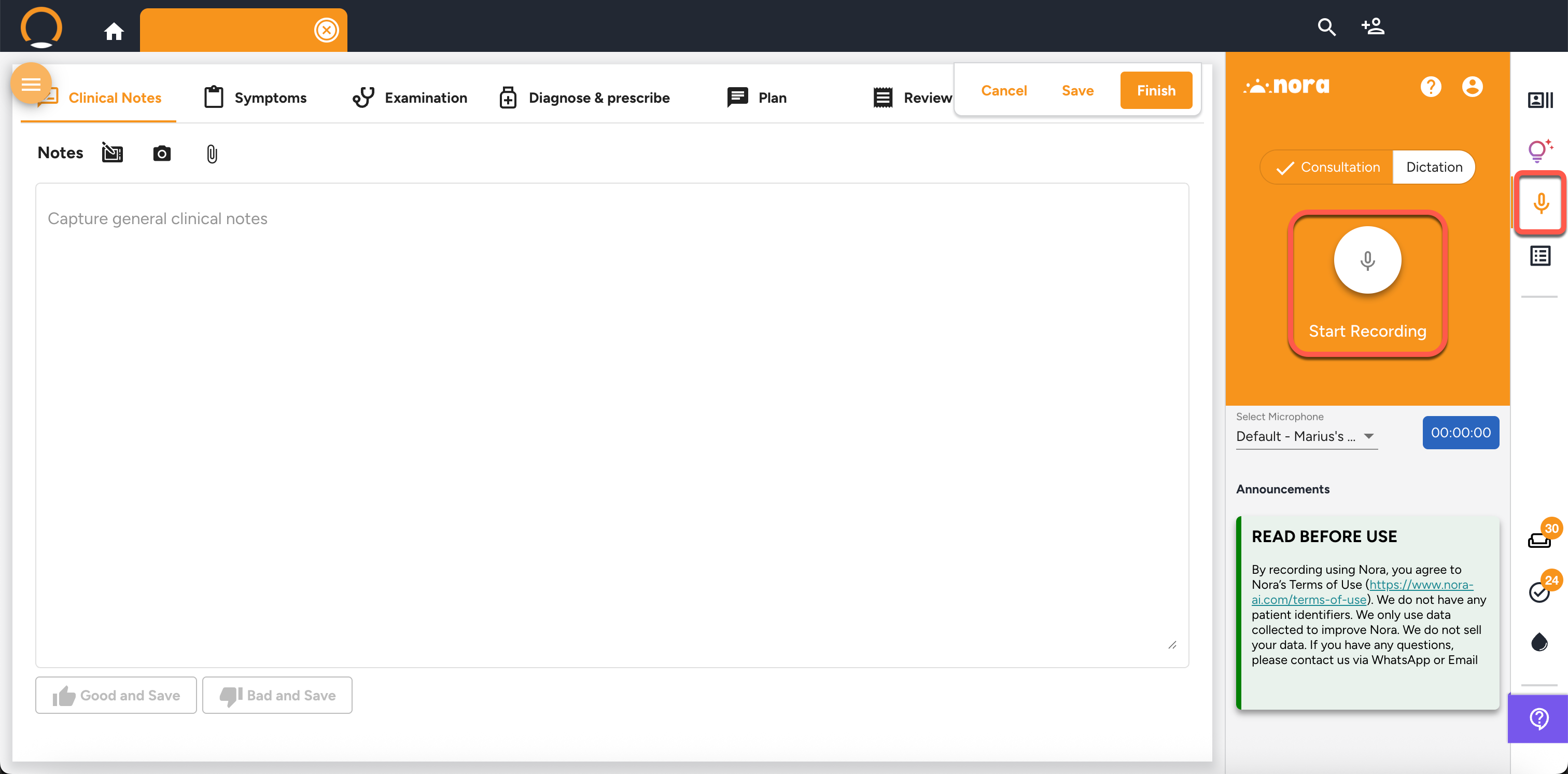
Note: Once you click 'Start Recording', Nora continues recording in the background as you move through all the consultation tabs — Symptoms, Examination, Diagnose & prescribe, and Plan. You do not need to stay on the Clinical Notes tab. Continue the consult as normal and Nora will capture everything until you click 'Stop Recording'. Narrate your physical examination findings aloud as you work (e.g. "Abdomen is soft, no tenderness") so they are captured in the structured note. Examination vitals must still be entered manually in the Examination tab. Nora supports English and Afrikaans only — place your device close to both you and the patient and speak clearly.
Step 4: Select the complaint and visit type on the Symptoms tab
Consultation — Symptoms tab
Click the 'Symptoms' tab. Under 'Complaint', click the relevant symptom buttons (such as 'Fever', 'Headache', or 'Cough'). Under 'Visit Type', click the type of consultation (such as 'General checkup' or 'Chronic follow up - Diabetes'). Selecting a complaint or visit type will prompt Healthbridge Clinical to generate customised examination questions.
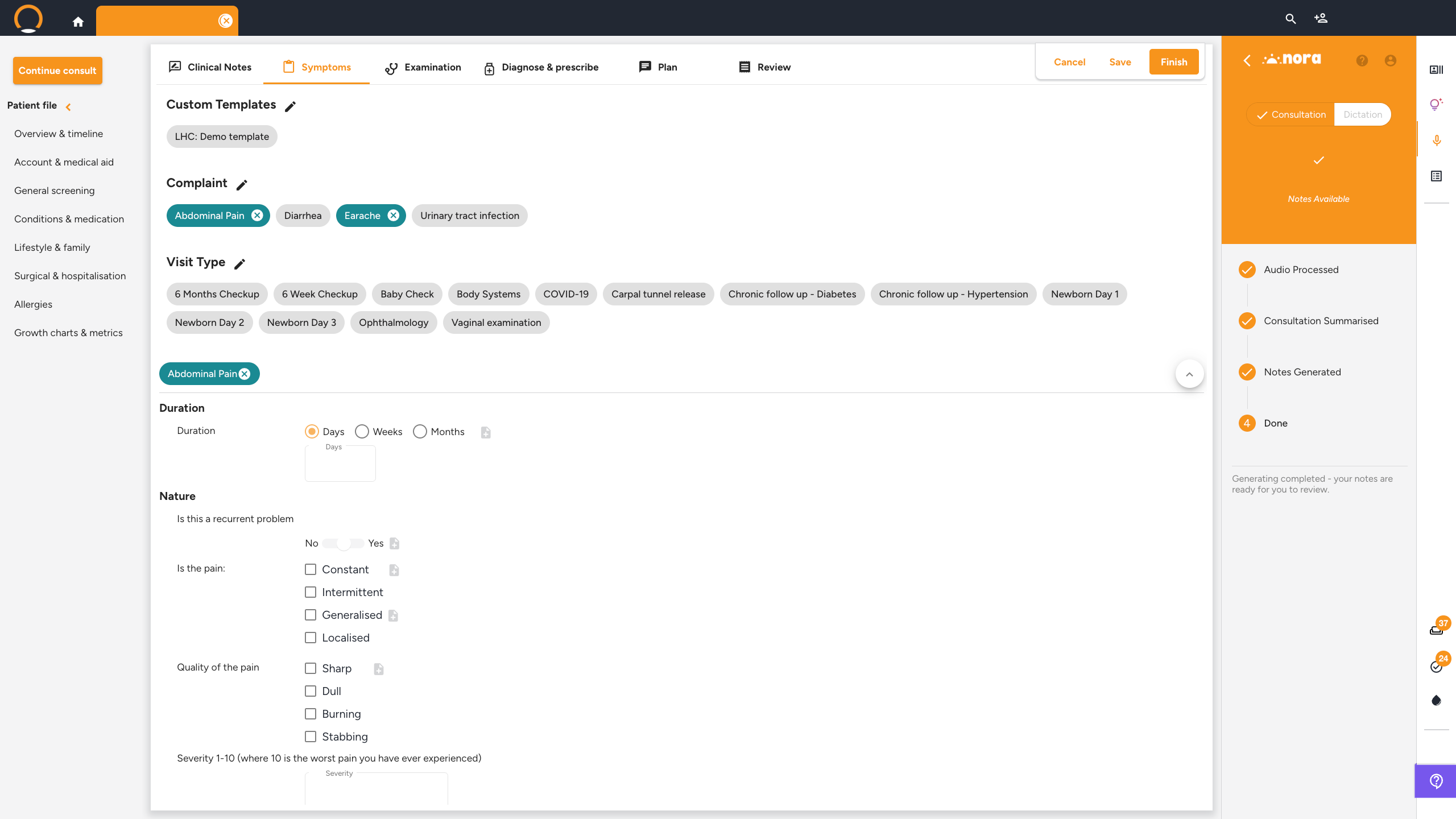
✓ You should see: the selected complaint or visit type is highlighted, and customised examination prompts may appear on the Examination tab.
Step 5: Record examination findings on the Examination tab
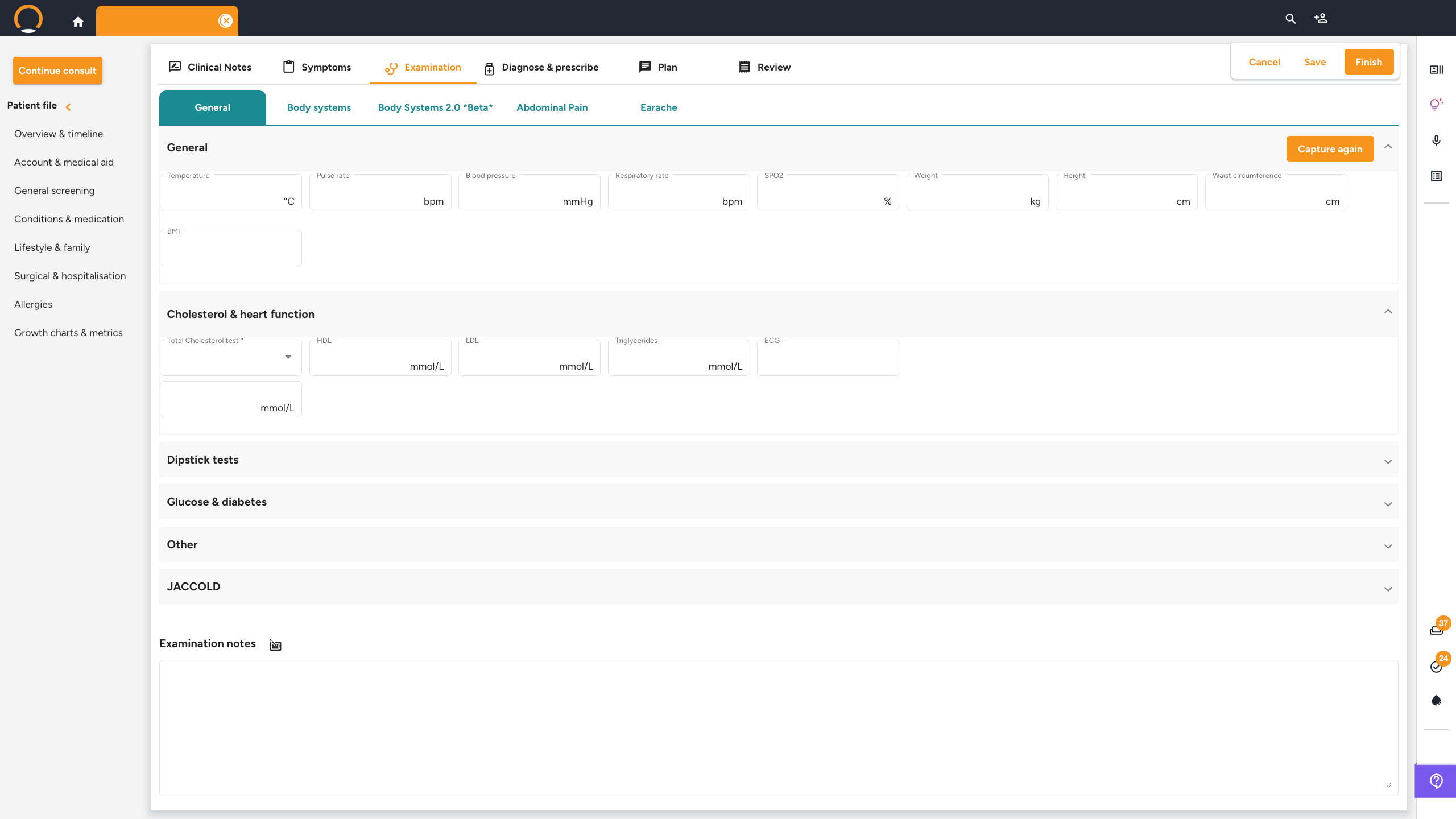
Consultation — Examination tab — General
Click the 'Examination' tab. On the 'General' sub-tab, enter the patient's vitals: Temperature, Pulse rate, Blood pressure, Respiratory rate, SPO2, Weight, Height, Waist circumference, BMI, Peak flow, and Head circumference. Additional measurement categories (Cholesterol & heart function, Dipstick tests, Glucose & diabetes, and more) are available as expandable sections below.
- Click 'Questionnaires' to administer structured clinical screenings (e.g. PHQ-9, GAD-7).
- Click 'Body systems' to document system-by-system examination findings using tick-box templates.
- Body Charts (🖊️) — click the Stylus icon in the sub-tab toolbar, then select 'Add Templates' to open a body diagram. Available charts include Full Body (Front/Back), Body Side View, Foot Chart, and Hand Chart. On touchscreens, draw directly on the diagram. On desktop, click the Textbox icon to insert typed annotations next to specific areas.
Step 6: Add diagnosis, medication, and procedures on the Diagnose & prescribe tab
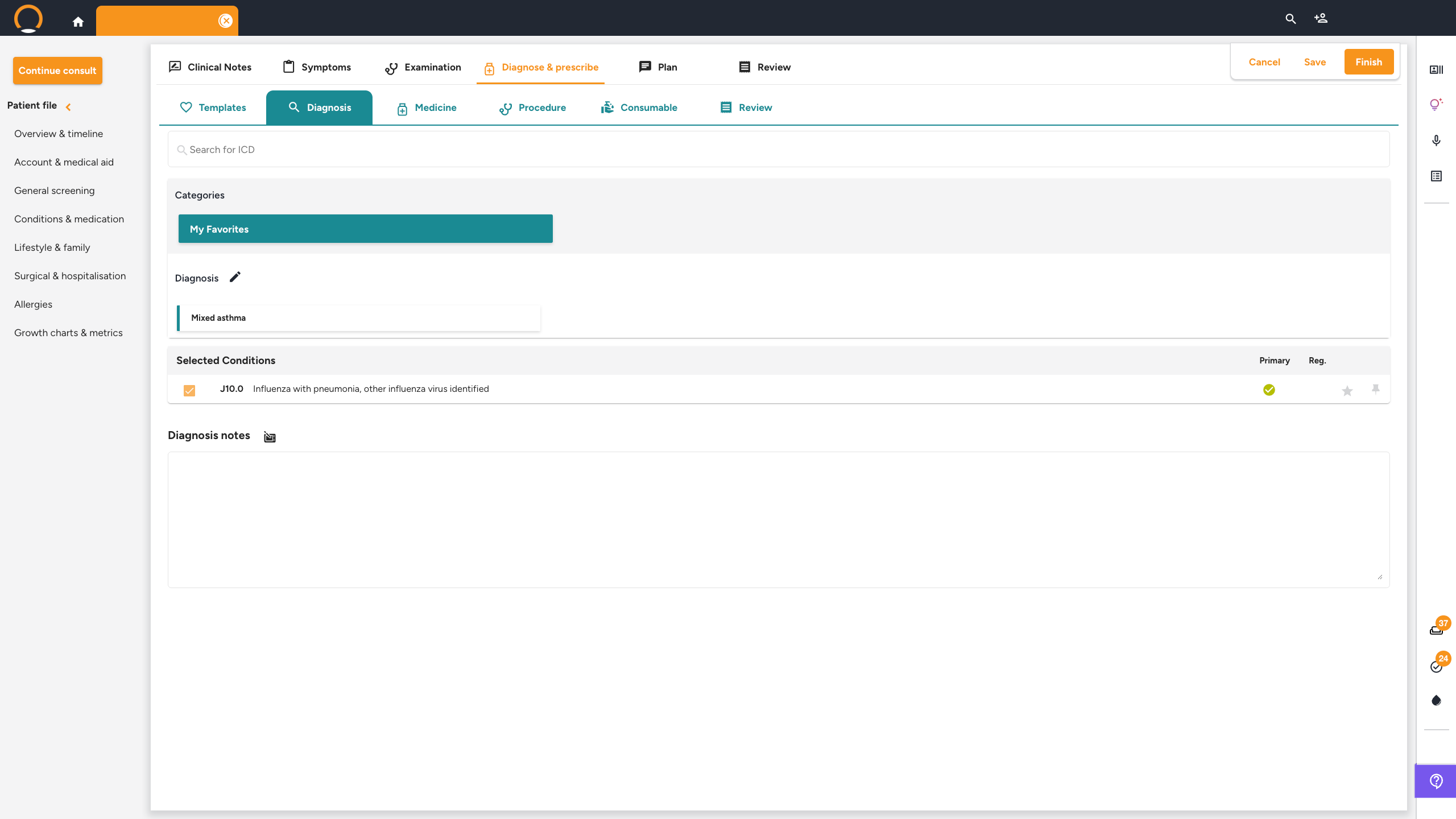
Consultation — Diagnose & prescribe tab
Click the 'Diagnose & prescribe' tab. Work through the sub-tabs from left to right:
- Templates — apply a saved consultation template if you have one set up.
- Diagnosis — search and add ICD-10 codes for the patient's diagnoses. Click the Star icon (★) next to any ICD-10 code to save it to your Favourites list for quick access in future consultations.
- Medicine — use SmartMeds to search for medication, check formulary and dosage, and add to the prescription. Click the Star icon (★) next to any medication name to save it to your Favourites. Once prescribed, watch for a Warning icon (⚠) appearing next to any line item — this indicates a detected drug-to-drug or drug-to-condition interaction. Click the warning icon to view the severity level, potential risks, and suggested alternative medications before confirming the prescription.
- Procedure — add any clinical procedures performed during the visit.
- Consumable — add any materials used (e.g. bandages, syringes).
- Review — review all line items before finalising.
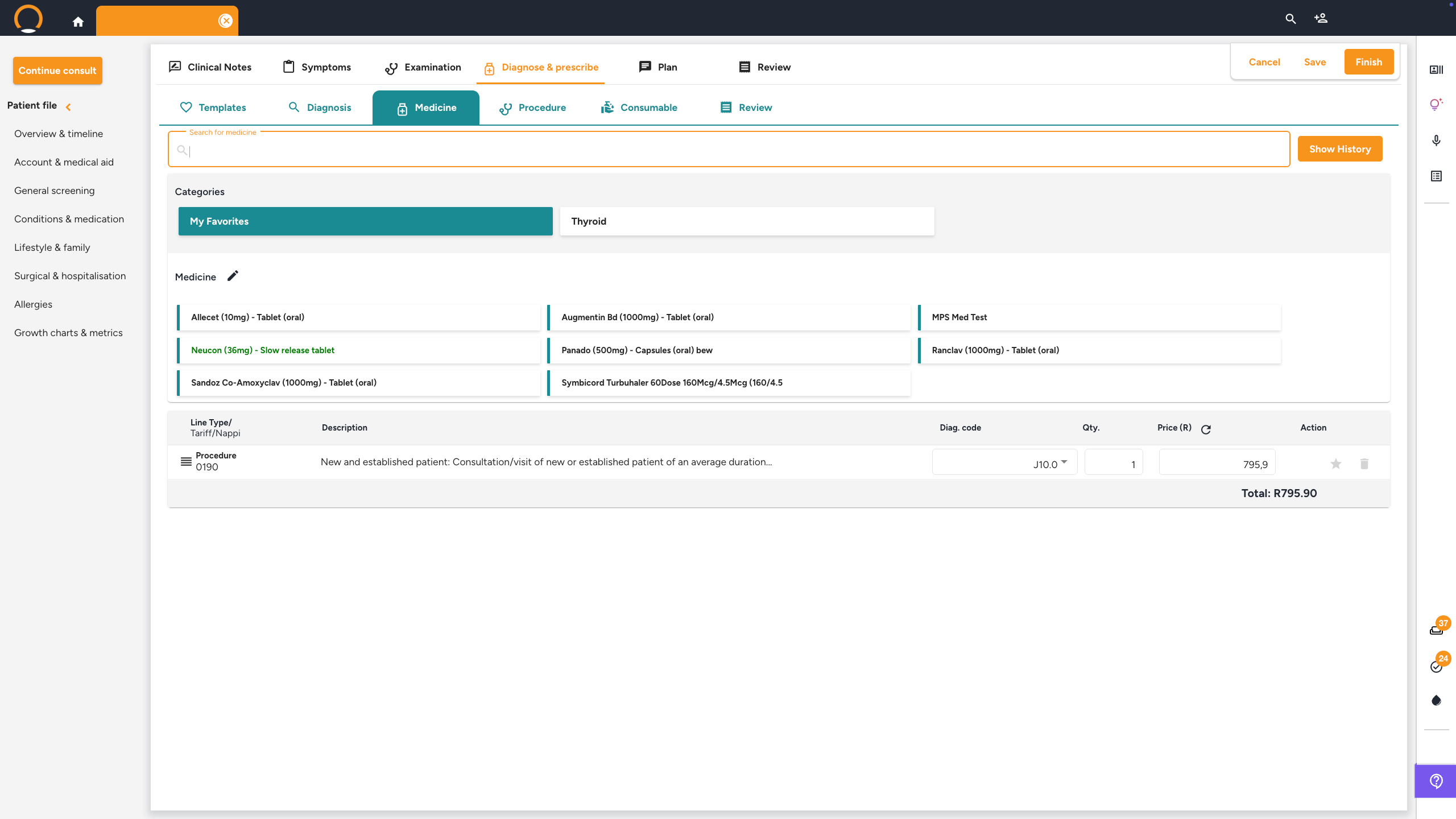
Tip: Always search for the ICD-10 code rather than typing free text. Selecting the correct ICD-10 code links the diagnosis to the prescription and procedures automatically, which streamlines medical aid billing.
Step 7: Use the Clinical Assistant to generate letters and documents
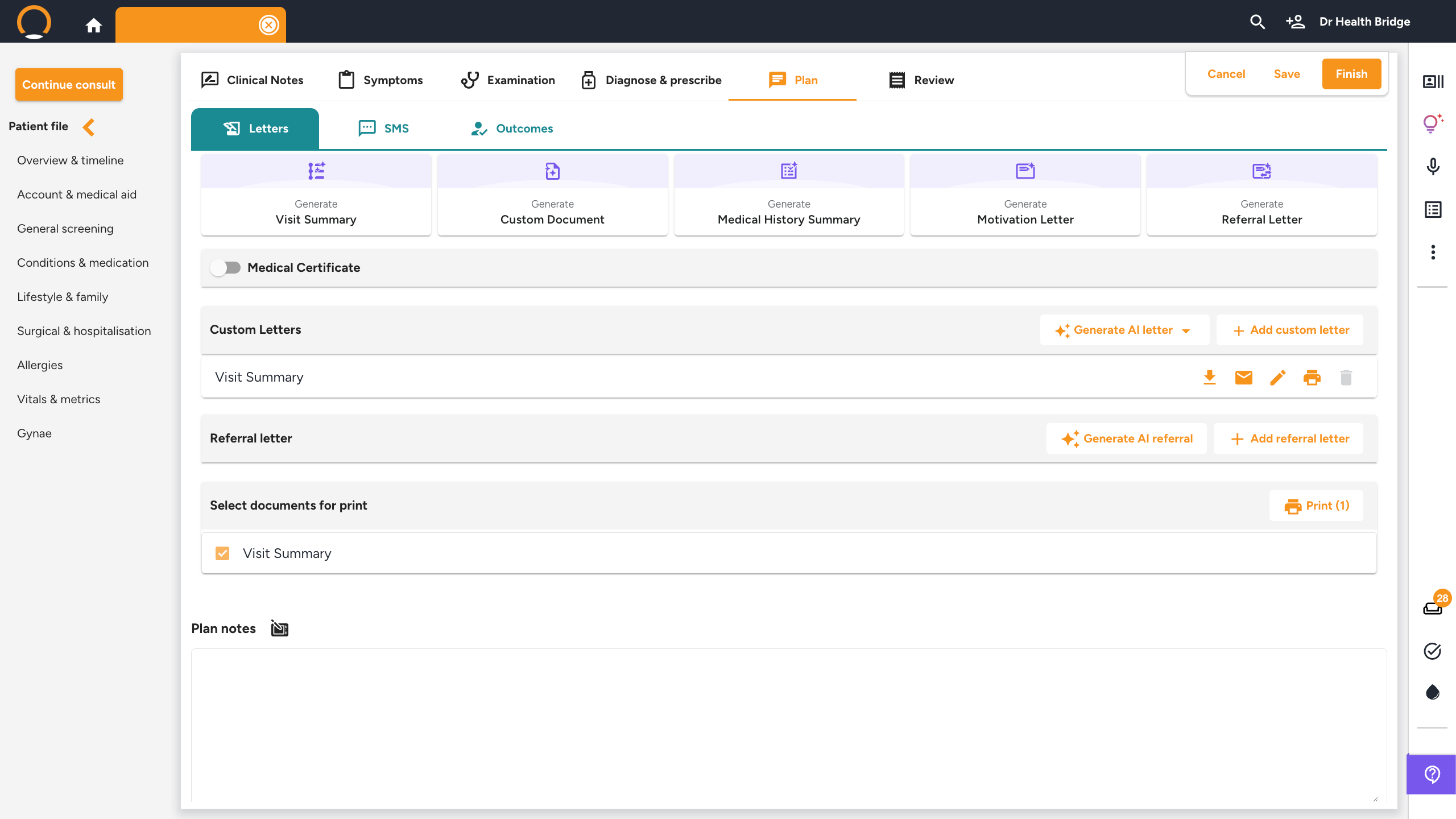
Consultation — Plan tab — Letters
The Clinical Assistant is an AI-powered documentation tool built into Healthbridge Clinical. It eliminates the administrative burden of writing letters, summaries, and referrals by automatically pulling relevant clinical data from the patient's entire history and producing professional, structured documents in seconds.
Advanced AI feature: The Clinical Assistant document generators require an Advanced AI subscription. Practices on the Core tier will not see these options. Nora (Speech to Clinical Notes) is a separate AI tool with its own subscription tiers.
Click the 'Plan' tab. On the 'Letters' sub-tab you will find five Clinical Assistant generators:
- Generate Visit Summary — translates your consultation notes into a clear, patient-friendly take-home guide in plain language, covering the diagnosis, treatment plan, and follow-up steps. Directly addresses the problem of patients forgetting what you told them. The summary is saved to the patient's timeline and can be sent via WhatsApp immediately after the consult. Example instruction: "Emphasise the importance of completing the full antibiotic course and include warning signs to watch for."
- Generate Custom Document — a flexible "do-anything" tool for creating unique letters or reports when standard templates don't fit. Describe what you need in plain language and the AI drafts it using the patient's file. Example instructions: "A letter to the school explaining the patient has ADHD and requires extra exam time" or "A medical clearance letter for airline travel with a portable oxygen concentrator."
- Generate Medical History Summary — compiles the patient's full medical journey into a professional, chronological narrative: diagnoses, treatments, hospitalisations, and significant events. Ideal for patient transfers, insurance requests, or specialist onboarding. You can scope it to a specific period. Example instruction: "Create a medical history summary for the past 3 years only."
- Generate Motivation Letter — builds a persuasive clinical case to justify care or secure medical aid approval. The AI searches the entire timeline for supporting evidence: relevant diagnoses, medication trials, lab trends, and clinical notes. Example instruction: "Motivation for chronic medication benefits for the patient's diagnosed asthma."
- Generate Referral Letter — drafts a structured specialist referral that intelligently curates the most relevant data for the receiving specialist: demographics, allergies, medications, history, and recent lab results, all tailored to the stated reason for referral. The completed letter is automatically saved to the patient's timeline. Example instruction: "Referral to a cardiologist for assessment of recurrent palpitations and chest pain."
All five generators share a single pop-up — click any card to open it:
- Click a generator card, the Clinical Assistant pop-up opens. At the top of the pop-up are tabs for all five document types; click any tab to switch type without reopening.
- In the 'Enter your instructions...' field, type what you need (the more specific, the better), then click 'Generate'. The AI drafts the document from the patient's timeline.
- Review the draft. If refinements are needed, type a follow-up instruction (e.g. "Make the tone more formal" or "Include the lab results from last month") and click 'Regenerate'.
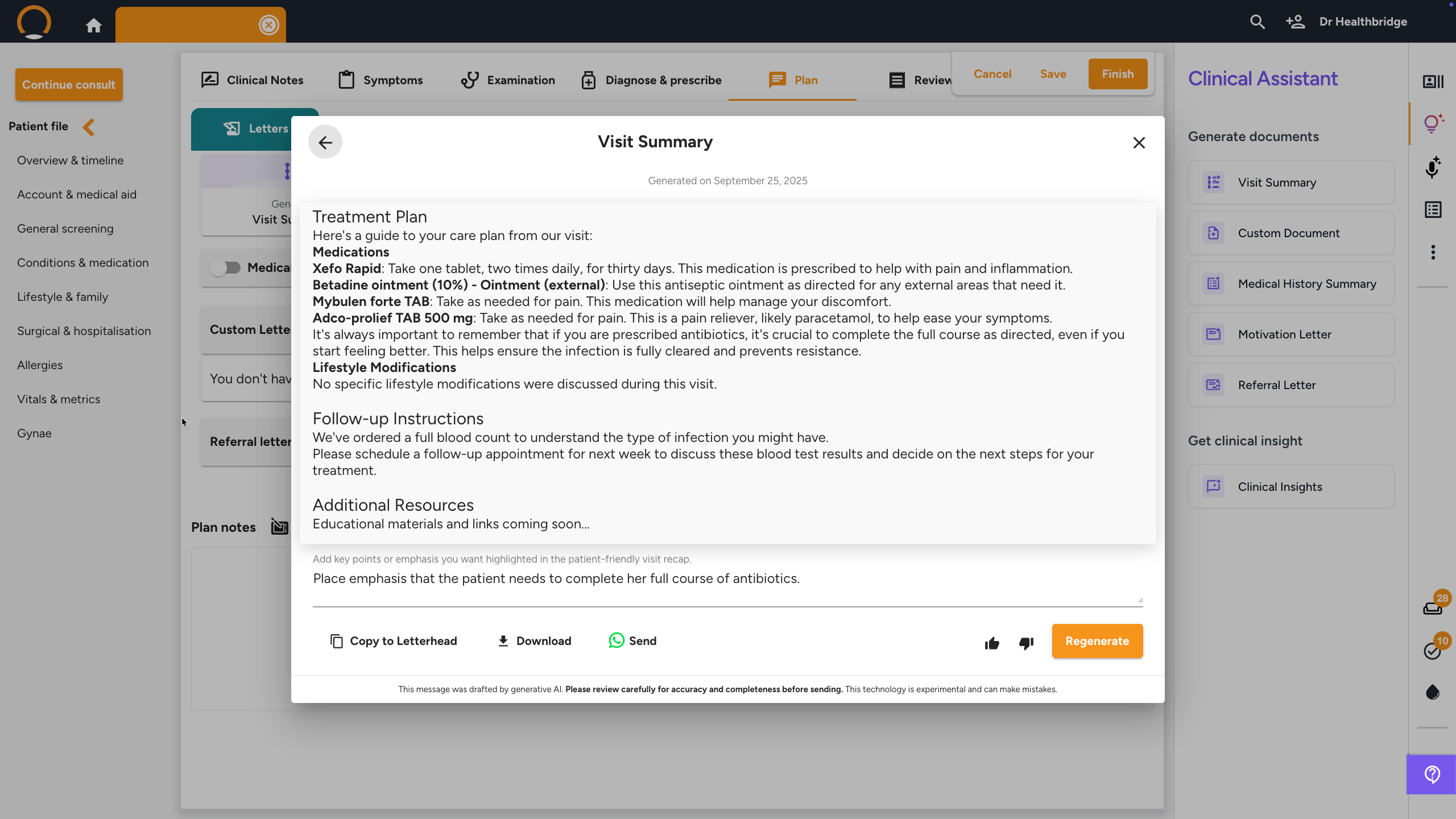
- Click 'Copy to Letterhead' to transfer the text onto your practice stationery.
- Click 'Send' (WhatsApp) to deliver directly to the patient's phone.
- Click 'Download' for a local PDF copy.
The Clinical Assistant is also available outside a consultation: from the Patient Overview, click the Lightbulb icon (💡) in the right-hand sidebar to access all five generators at any time, useful for producing documents after the patient has left.
If you prefer to write documents manually without AI assistance, scroll down below the five generator cards:
- Under 'Custom Letters', click '+ Add custom letter' to open a blank template and type your own content.
- Under 'Referral letter', click '+ Add referral letter' to select a specialist from the Address Book and draft a referral manually.
To issue a Medical Certificate, toggle the switch to 'On'. Use 'Plan notes' at the bottom for additional follow-up instructions.
✓ You should see: the Clinical Assistant pop-up shows the generated document. Review and refine the text before distributing via letterhead, WhatsApp, or download.
Step 8: Review the invoice, send to admin, and click Finish
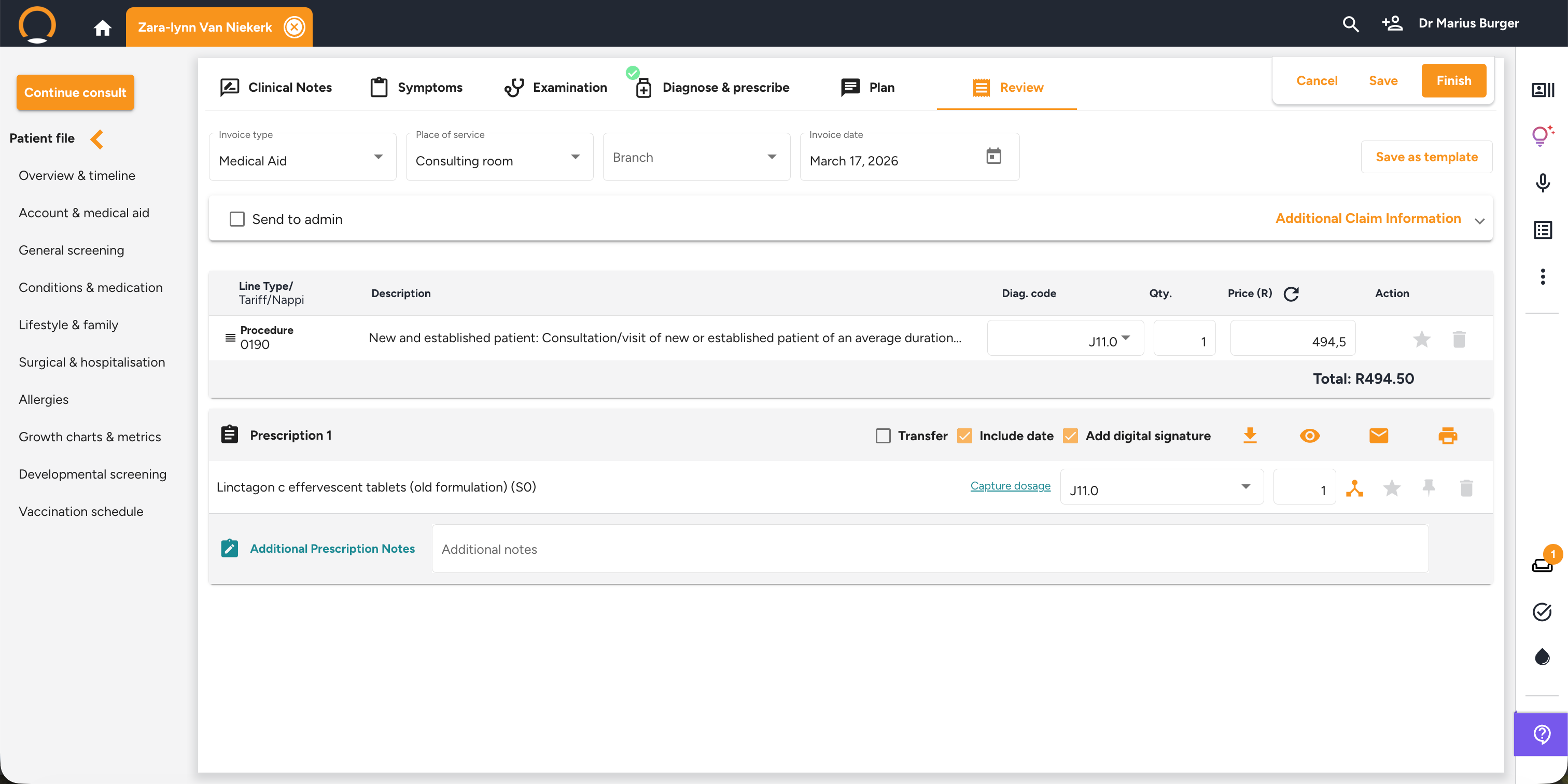
Consultation — Review tab
Click the 'Review' tab (last tab in the consultation navigation). Verify the invoice line items, invoice type, and place of service. Then choose how to finalise:
- Tick 'Send to admin' to route the invoice to your practice administrator's inbox for review and medical aid submission.
- Click the orange 'Finish' button to close the consultation. The notes are locked and the full encounter is saved to the patient's timeline.
- Click 'Save' (or close the file) if you want to pause and continue later, the consultation will remain open and can be resumed by opening the patient file and clicking 'Continue consult'.
FAQ
Can I save a consultation mid-way and come back to it?
Yes. Click 'Save' or simply close the patient file. When you re-open the patient file later, the button will show 'Continue consult', clicking it resumes the consultation exactly where you left off.
Can I move on to the next patient before finishing the invoice?
Yes. Complete your clinical notes and plan, then click Finish. The consultation moves to the admin inbox where your receptionist can add consumables, review procedures, and submit the invoice, without needing access to Healthbridge Clinical itself.
Will Nora fill in the Examination tab automatically when I dictate?
No. Nora captures your dictation in the Clinical Notes tab only. Vitals and examination findings in the Examination tab must be entered manually. You can, however, include examination details in your Clinical Notes dictation for the record.
Can I have multiple patient files open at the same time?
Yes. You can open multiple patient files simultaneously and toggle between them. Each file retains its state, so you can consult with different patients across the day without closing and reopening files.
Can I capture clinical notes without generating a bill?
Yes. Complete the Clinical Notes tab and any other tabs you need, then click Finish without entering anything in the Diagnose & prescribe tab. No invoice will be generated, and the notes are saved to the patient's timeline as normal.
Do I need a specific subscription to use the Clinical Assistant document generators?
Yes. The five Clinical Assistant generators (Visit Summary, Custom Document, Medical History Summary, Motivation Letter, and Referral Letter) are part of the Advanced AI subscription tier. Practices on the Core tier will not see these options in the Plan tab. Nora (Speech to Clinical Notes) is a separate AI tool managed under its own subscription tiers (Lite, Premium, and Pro).
What instructions should I give when using a Clinical Assistant generator?
Be as specific as possible. Include the purpose of the document, who it is for, and any particular details you want emphasised or included. For example, rather than clicking Generate on a blank instruction field for a referral letter, write: "Referral to a cardiologist for assessment of recurrent palpitations and chest pain, please include the ECG results from last month." The AI curates the patient's timeline based on your instruction, a richer prompt produces a richer document. If the first draft is not right, use the instruction field to refine it and click Regenerate.